
iHealthBrokers | Medigap
A Medigap policy is private health insurance that helps supplement Original Medicare. This means it helps pay some of the health care costs that Original Medicare doesn’t cover (like copayments, coinsurance, and deductibles). These are “gaps” in Medicare coverage. If you have Original Medicare and a Medigap policy, Medicare will pay its share of the Medicare-approved amounts for covered health care costs. Then your Medigap policy pays its share. A Medigap policy is different from a Medicare Advantage Plan (like an HMO or PPO) because those plans are ways to get Medicare benefits. In contrast, a Medigap policy only supplements the costs of your Original Medicare benefits. Note: Medicare doesn’t pay any of your expenses for a Medigap policy.
All Medigap policies must follow federal and state laws designed to protect you, and policies must be identified as “Medicare Supplement Insurance.” Medigap insurance companies in most states can only sell you a “standardized” Medigap policy identified by letters A through N. Each standardized Medigap policy must offer the same essential benefits, no matter which insurance company sells it. Cost is usually the only difference between Medigap policies with the same letter sold by different insurance companies.
In Massachusetts, Minnesota, and Wisconsin, Medigap policies are standardized in a different way. In some states, you may be able to buy another type of Medigap policy called Medicare SELECT. Medicare SELECT plans are standardized plans that may require you to see certain providers and may cost less than other plans.
This chart shows basic information about the different benefits that Medigap policies cover. If a percentage appears, the Medigap plan covers that use percentage, and you must pay the rest.
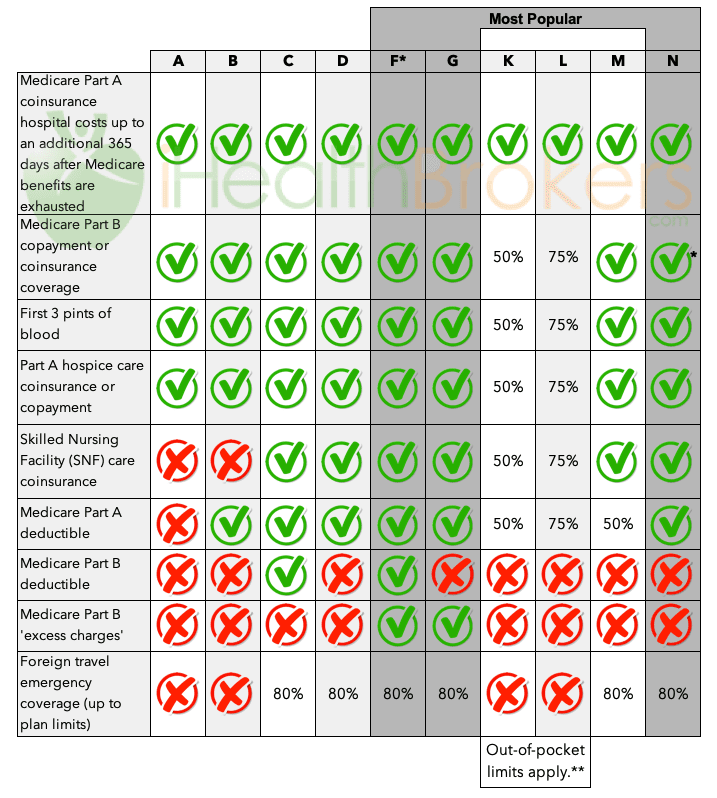
*Plan F is also offered as a high-deductible plan. With a high-deductible Plan F, you must pay for Medicare-covered expenses such as copays and deductibles up Plan deductible of $2,490 for 2022 before the policy pays anything.
*Plan N covers Basic Benefits after a $20 copay for office visits and a $50 copay for emergency room visits.
**Plans K and L pay 100% of hospitalization and preventive care Basic Benefits. All other Basic Benefits are paid at 50% for Plan K and 75% for Plan L. Once you reach the annual limit, the plan pays 100% of the Medicare copayments, coinsurance, and deductibles for the rest of the calendar year. The yearly out-of-pocket limit does NOT include costs from your provider that exceed Medicare-approved amounts (excess charges). For 2019, the out-of-pocket will be $6,220 for Plan K and $3,110 for Plan L.
Medicare Supplement plans are offered by private insurance companies. They’re meant to help with some of the out-of-pocket health care costs associated with Original Medicare, such as copayments, coinsurance, and deductibles. There are 10 different Medicare supplements—plans A, B, C, D, F, G, K, L, M, and N. Each offers its own variety of benefits at relative costs for personalized coverage.
The reason why Medicare Supplement Insurance (or Medigap) plans cover the many out-of-pocket costs you face with Original Medicare is that, on their own, Parts A and B offer decent, low-cost coverage, but they certainly don’t cover everything.
Besides Medigap, your other additional options include Medicare Advantage and Part D. Unlike Medicare Advantage, which is a full alternative to Original Medicare that includes all of its coverage in a newly structured plan with some additional benefits, supplements are, as the name implies, a “supplement.”
Medigap is an addition to coverage options rather than an alternative. This, however, does not mean that you will be paying more—in fact, you will be saving a significant amount on Original Medicare with a supplement plan. Keep in mind though, that you can’t be joined in a Medicare Prescription Drug Coverage plan and have a Medigap policy with drug coverage. This means that if you already have an existent Medigap policy that covers prescription drugs, you’ll need to tell your Medigap insurance company if you join a Medicare Prescription Drug Plan. The Medigap insurance company will then remove the prescription drug coverage from your Medigap policy and adjust your premium.
All supplement plans offer this coverage:
Part A Coinsurance & Hospital Costs
Part B Coinsurance or Copayment
First 3 Pints of Blood for Transfusions
Part A Hospice Care Coinsurance or Copayment
The most basic of all the supplement plans is Plan A. All 10 options offer these minimal benefits. The more benefits are added, the more it will cost monthly. However, even as your monthly cost increases, you will still be saving a significant amount on your Original Medicare coverage.
This is where your decision on a plan becomes important. Yes, you will pay a higher monthly premium for more coverage, but you will also be paying much less out-of-pocket for the healthcare you receive.
Some plans, like Plan K, offer a percentage of benefits to lower your monthly costs:
100% of Part A Coinsurance and Hospital Costs
50% of Part B Coinsurance/Copayment
50% of the First 3 Pints of Blood for Transfusions
50% of Part A Hospice Care Coinsurance or Copayment
50% of Skilled Nursing Care Facility Coinsurance
50% of the Part A Deductible
This way, you know that you are still getting coverage with only half of the total cost coming out of your wallet.
Other plans, like Plan F, offer the fullest possible coverage at a higher monthly cost:
Part A Coinsurance & Hospital Costs
Part B Coinsurance/Copayment
First 3 Pints of Blood for Transfusions
Part A Hospice Care Coinsurance/Copayment
Skilled Nursing Care Facility Coinsurance
Part A Deductible
Part B Deductible
Part B Excess Charges
80% of Foreign Travel Emergency Care
Keep in mind that Medicare Plan F is not available anymore to some extent. Due to a change in federal law, people who have become eligible for Medicare after December 31, 2019. do not qualify for Plan F. However, Plan F continues to be available to everyone who became eligible for Medicare before that date.
No matter which one of the plans you choose to enroll in, you will save a lot of money on your Original Medicare coverage. Check out our Medicare Supplement Plan Comparison to review your full options and choose a supplement that works best for you.
If you have chosen a supplement plan, your next step is to enroll. The best time to do so is during your Medigap General Enrollment Period (GEP).
During the 7 months following your 65th birthday, you can enroll in any Medigap plan without fear of being turned away due to your health. After the General Enrollment Period, it may be harder to enroll but still possible in case you have a medical condition.
Another option you have is to simply enroll during your Medigap Open Enrollment Period. It is during this time that you can buy any Medigap policy sold in your state, even if you have health problems, and will generally get better prices and more choices among policies. This period automatically starts the first month you get your Medicare Part B (Medical Insurance) and you’re 65 years old or older. This time period can’t be changed or repeated and after the period ends, you may not be able to buy a Medigap policy. If you’re able to buy one, it may cost more due to past or present health problems.
Taking all this into consideration, we typically advise that you enroll in one as soon as you are able.








Insurance sold on iHealthBrokers.com is processed through the licensed entity: Smedley Insurance Group, Inc.
We may not offer every Medicare plan available in your area. Any information we provide is limited to those plans we do offer in your area.
Please contact Medicare.gov or 1-800-MEDICARE to get information on all of your options.
We are not connected with or endorsed by the United States government or the federal Medicare program.